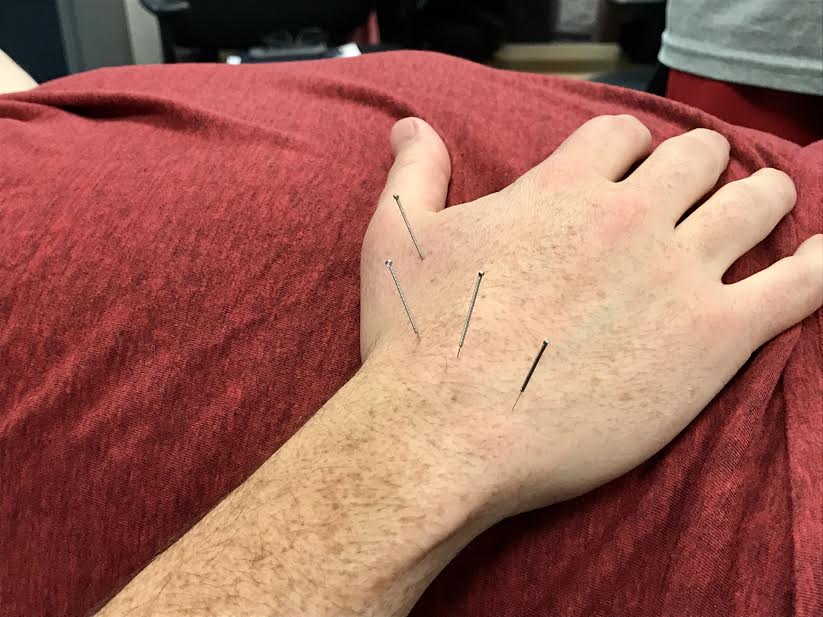
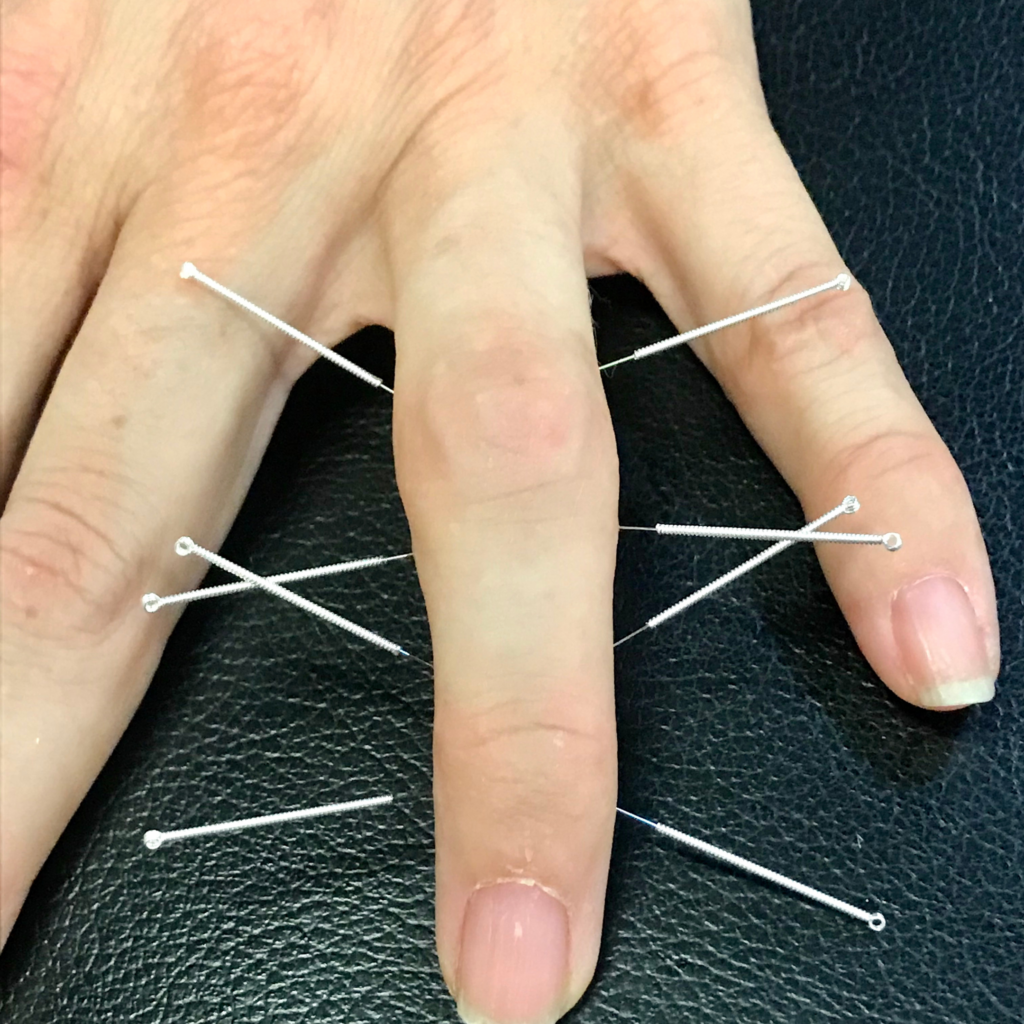
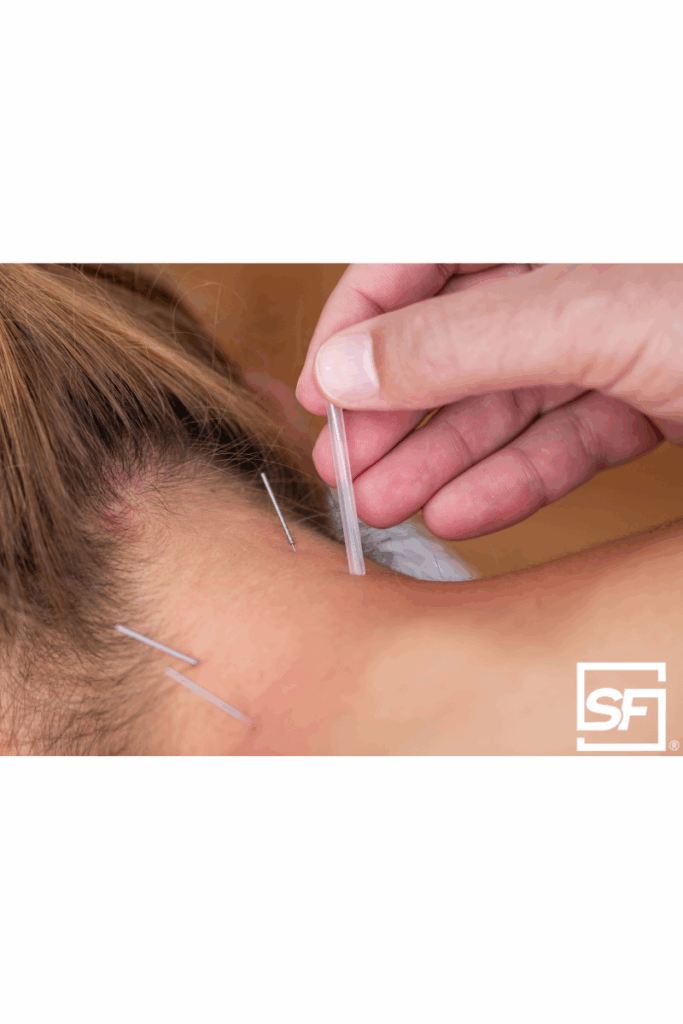
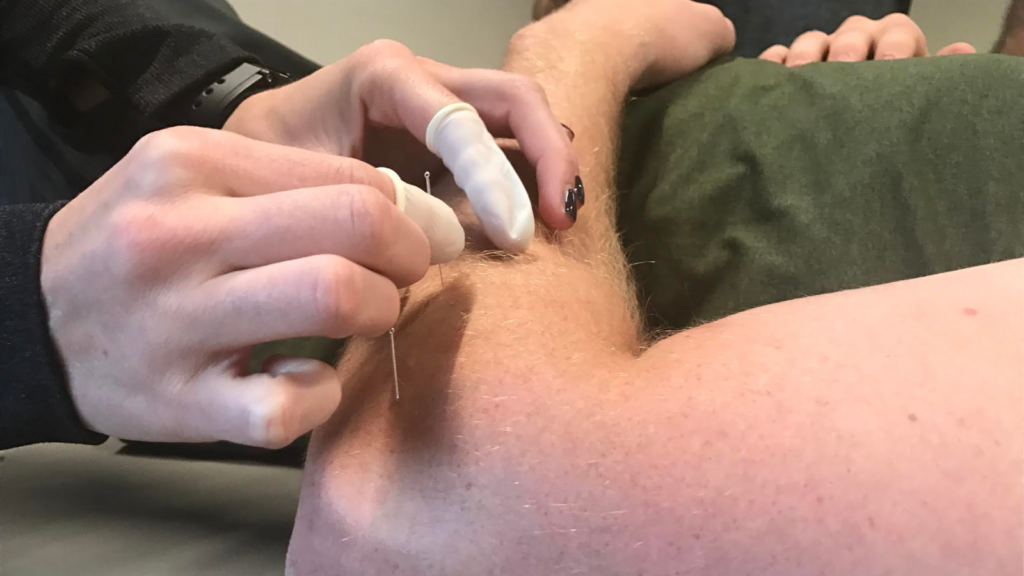
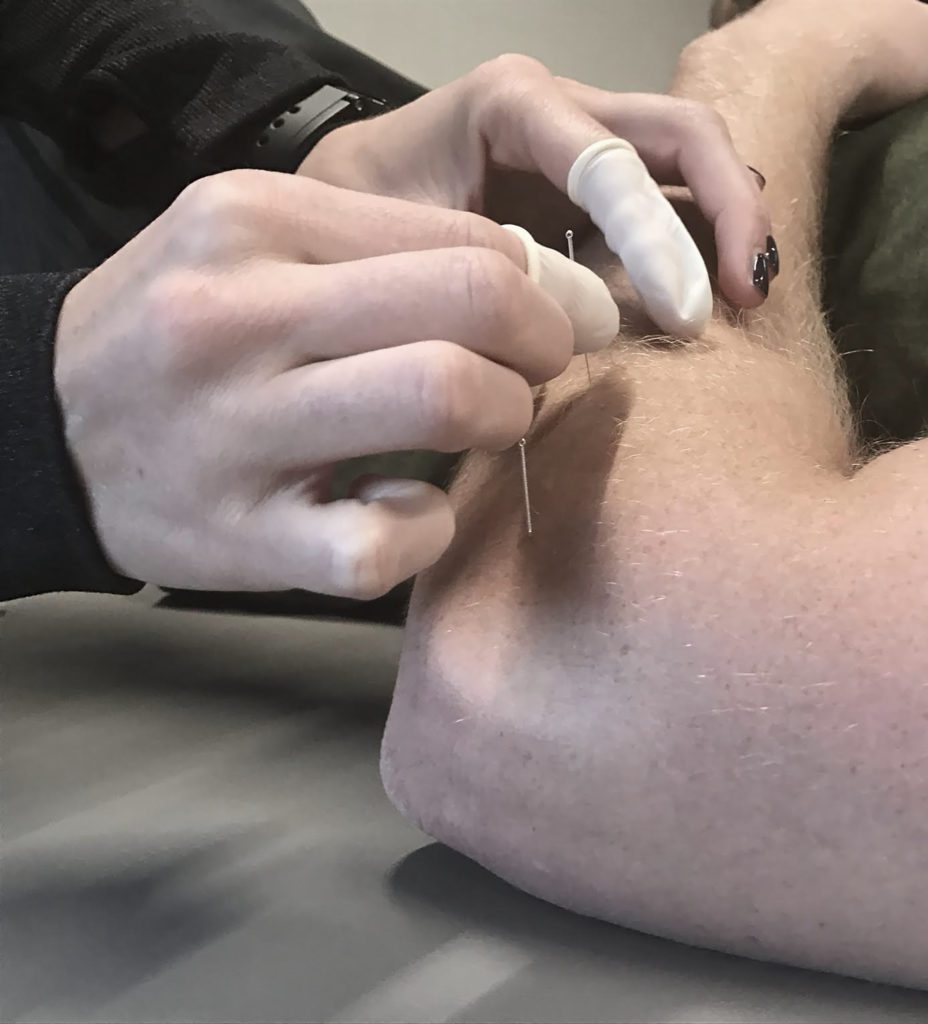
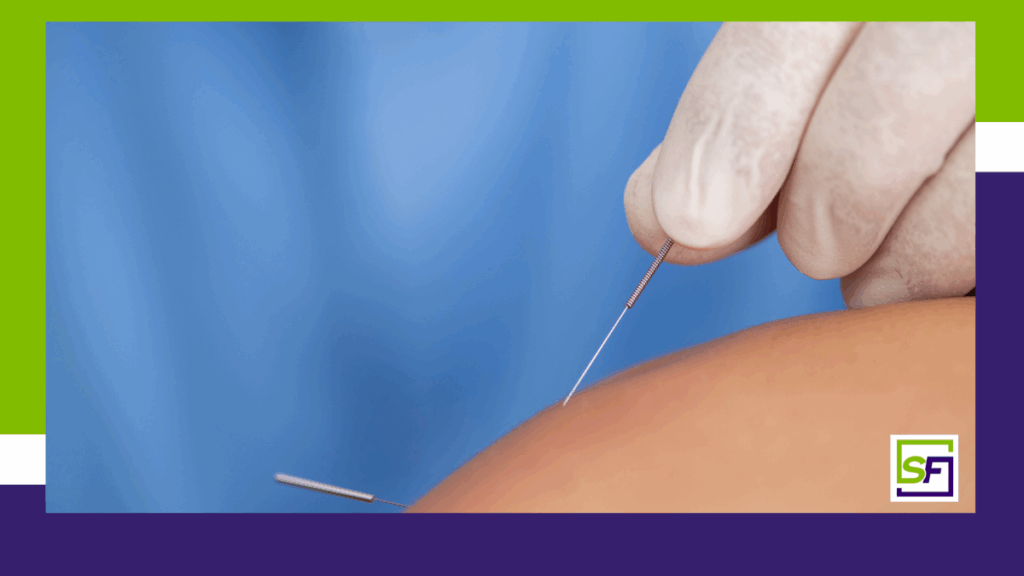
Beyond the Needle: Unveiling the Advanced Neurobiology of Electroacupuncture (EA) and Electro-Dry Needling (EDN) for Enhanced Clinical Outcomes
Enhance your dry needling practice. Investigate the innovative neurobiological principles, exact dose specifications, and sophisticated clinical uses of electroacupuncture (EA) and electro-dry needling (EDN) for chronic, neuropathic, and inflammatory pain, based on contemporary research. As clinicians dedicated to evidence-based therapy and advancing musculoskeletal intervention, we consistently pursue methods that provide not only clinical relief but […]