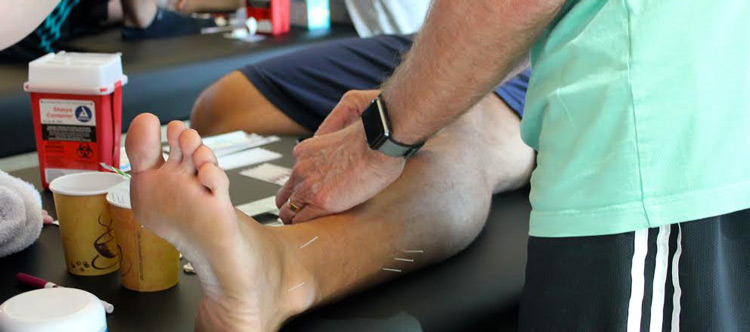
Multimodal Approaches to Treating Lumbopelvic Pain in Women
Welcome to Women’s Health Month! This month, we celebrate women’s incredible strength, resilience, and vitality everywhere. It’s a time to prioritize your well-being and take proactive steps toward better health. Women often prioritize the health of those around them, but focusing on their needs is equally important. One common condition women suffer from is lumbopelvic pain, particularly after pregnancy. In my opinion, a significant hole in our medical system is adequate postpartum care for females suffering negative consequences of childbirth. Lumbopelvic pain is a substantial concern among postpartum females. As therapists, it’s crucial to employ a comprehensive approach to address this discomfort effectively. In this blog post, we’ll explore various treatment modalities, including dry needling, fascial manipulation, and joint manipulation approaches, to provide relief and enhance the overall well-being of our patients.
Understanding the Prevalence and Etiology of Pelvic Pain in Women:
Pelvic pain is a prevalent issue among women, with studies indicating that up to 20% of women experience chronic pelvic pain at some point in their lives. Within the postpartum population, the prevalence of pelvic pain can be even higher, affecting approximately 25-30% of women in the months following childbirth.1
The etiology of pelvic pain in women can be multifactorial, often stemming from a combination of anatomical, physiological, and psychosocial factors. In many cases, pelvic pain is linked to conditions such as endometriosis, pelvic inflammatory disease, uterine fibroids, or interstitial cystitis. Additionally, musculoskeletal issues, including lumbopelvic dysfunction and pelvic floor dysfunction, can contribute to the development of pelvic pain, especially in the postpartum period.1-3
Childbirth-related trauma, such as perineal tears, episiotomies, or pelvic floor muscle injuries, can also play a significant role in the onset of pelvic pain postpartum. Changes in hormone levels during pregnancy and lactation may further exacerbate pelvic pain symptoms, affecting the musculoskeletal and nervous systems.4
It’s essential for therapists to consider the complex interplay of all of these potential factors when assessing and treating pelvic pain in women. A thorough evaluation, including a detailed medical history and physical examination, can help identify the underlying causes of pelvic pain and guide the development of individualized treatment plans.
By addressing both the physical and emotional aspects of pelvic pain, therapists can provide holistic care that promotes healing and enhances the overall well-being of women experiencing this debilitating condition.4 Through targeted interventions and ongoing support, we can empower women to regain control of their pelvic health and live fulfilling, pain-free lives.
Treatment Approaches for Pelvic Pain in Women:
Addressing pelvic pain often requires a multimodal approach that combines various treatment modalities to target different aspects of the condition. This may include a combination of pharmacological interventions, focused therapy, and complementary therapies such Fascial Manipulation® and dry needling.
Therapy is crucial in managing pelvic pain by addressing musculoskeletal imbalances, improving pelvic floor function, and promoting overall mobility and strength. Targeted exercises to strengthen the core, stabilize the pelvis, and improve posture can help reduce pelvic pain and prevent recurrence. These exercises may include pelvic tilts, bridges, abdominal bracing, and pelvic floor exercises. Pelvic floor rehabilitation is typically indicated as pelvic floor muscle dysfunction is a common contributor to pelvic pain in women. Pelvic floor physical therapy aims to restore the optimal function of these muscles through exercises, manual therapy, biofeedback, and relaxation techniques.5
Manual therapy techniques such as the Fascial Manipulation® method can also be effective.
The key concept of the Fascial Manipulation® method is that a correct tension of the pelvic fasciae can be obtained by also treating distant fasciae, resulting in relief of pelvic pain. The Fascial Manipulation® treatment is specific for each person, based on the symptoms and the clinical history. Recently, evidence has demonstrated this technique to be effective for managing pelvic pain.6
Joint manipulation/mobilization can also be effective for treating pelvic pain. These manipulation techniques used to improve the mobility of pelvic joints. It plays a vital role in pelvic floor manual therapy and can be highly effective in restoring flexibility and function. By targeting specific areas of stiffness or restriction, this method enhances the range of motion and alleviates discomfort. Gentle mobilization techniques may improve the mobility and alignment of the pelvis and surrounding joints, reducing strain on muscles and alleviating pain.7-8
Dry needling is gaining popularity as an effective technique for alleviating lumbopelvic pain in women.9-12 Dry needling encompasses the insertion of solid filament, non-injectate needles into, alongside or around muscles, nerves or connective tissues with or without mechanical and/or electrical stimulation to manage pain and dysfunction in neuromusculoskeletal conditions. Dry needling may address hypersensitive neural structures and spinal segments, enhance treatment of myofascial pain and trigger points in the pelvic floor and surrounding musculature, and assist in the facilitation and/or inhibition of abnormal muscle tone and motor recruitment patterns.9-12. Ultimately, dry needling can facilitate a more balanced resting tone, healthy motor recruitment patterns, and optimal neuromuscular utility to re-establish ideal function in pelvic pain patients.
Complementary Strategies for Long-Term Management:
In addition to hands-on treatment techniques, therapists can empower patients to actively manage their lumbopelvic pain. This may involve prescribing targeted exercises to strengthen core muscles, improve posture, and enhance overall stability. Furthermore, educating patients about ergonomic principles and lifestyle modifications can help prevent future flare-ups and promote a sustainable recovery journey.
We’ve created a quick handout show casing how to combating pelvic pain with a multimodal approach. The handout highlights the five major modalities to discuss with a patient.
Conclusion
Treating lumbopelvic pain in women requires a multifaceted approach that addresses both the physical and emotional aspects of the condition. By incorporating techniques such as dry needling, Fascial Manipulation®, and joint manipulation approaches into comprehensive treatment plans, therapists can provide effective relief and empower patients to reclaim their quality of life. By combining various treatment modalities, healthcare providers can help women effectively manage pelvic pain and improve their quality of life. Structure & Function Education has several curricular offerings to help you better treat pelvic pain. If you’re interested in learning how Structure & Function Education’s Pentamodal Method of dry needling can help you treat your patients with pelvic pain, enroll today in Foundations in Dry Needling for Orthopedic Rehab & Sports Performance and then learn more in our advanced course for the Lumbo-Pelvic-Hip Complex region. If you are interested in hands-on manipulative therapies to treat pelvic pain, we also have courses for you with our Foundations of Joint Manipulation by Fix Medical Group (JMN1) course and the Fascial Manipulation® Method by Stecco (FM) course. Learn more about us and our programs at structureandfunction.net.
References
- [Pubmed] Ahangari A. Prevalence of chronic pelvic pain among women: an updated review. Pain Physician. 2014 Mar-Apr;17(2):E141-7. PMID: 24658485.
- [Pubmed] Peinado Molina RA, Hernández Martínez A, Martínez Vázquez S, Martínez Galiano JM. Influence of pelvic floor disorders on quality of life in women. Front Public Health. 2023 Oct 24;11:1180907. doi: 10.3389/fpubh.2023.1180907. PMID: 37942254; PMCID: PMC1062
- [Pubmed] Sewell M, Churilov L, Mooney S, Ma T, Maher P, Grover SR. Chronic pelvic pain – pain catastrophizing, pelvic pain and quality of life. Scand J Pain. 2018 Jul 26;18(3):441-448. doi: 10.1515/sjpain-2017-0181. PMID: 29794266.
- [Pubmed] Verstraete EH, Vanderstraeten G, Parewijck W. Pelvic Girdle Pain during or after Pregnancy: a review of recent evidence and a clinical care path proposal. Facts Views Vis Obgyn. 2013;5(1):33-43. PMID: 24753927; PMCID: PMC3987347.
- [Pubmed] Curillo-Aguirre CA, Gea-Izquierdo E. Effectiveness of Pelvic Floor Muscle Training on Quality of Life in Women with Urinary Incontinence: A Systematic Review and Meta-Analysis. Medicina (Kaunas). 2023 May 23;59(6):1004. doi: 10.3390/medicina59061004. PMID
- [Publisher] PASINI A, SFRISO M, STECCO C. Treatment of chronic pelvic pain with Fascial Manipulation®. 2016; 35(1): 13-16
- [Pubmed] Bishop MD, Bialosky JE, Alappattu MJ. Riding a Tiger: Maximizing Effects of Manual Therapies for Pelvic Pain. J Womens Health Phys Therap. 2020 Jan-Mar;44(1):32-38. doi: 10.1097/jwh.0000000000000156. PMID: 34163308; PMCID: PMC8218714.
- [Pubmed] Barbosa AC, Martins FL, Barbosa MC, Dos Santos RT. Manipulation and selective exercises decrease pelvic anteversion and low-back pain: a pilot study. J Back Musculoskelet Rehabil. 2013;26(1):33-6. doi: 10.3233/BMR-2012-0347. PMID: 23411646.
- [Pubmed] Dydyk AM, Gupta N. Chronic Pelvic Pain. [Updated 2023 Apr 1]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK554585/
- [Pubmed] Chou L, Kao M, Lin J. Probably mechanisms of needling therapies for myofascial pain control. Evidence-Based Complimentary and Alternative Medicine. 2012;705327
- [Publisher] George, Alyssa PT, DPT, OCS1; VanEtten, Lucas PT, DPT, OCS2; Briggs, Matt PT, DPT, PhD, AT, SCS3. Dry Needling for Female Chronic Pelvic Pain: A Case Series. Journal of Women’s Health Physical Therapy 42(1):p 8-16, January/April 2018. | DOI: 10.1097/JWH.0
- [Pubmed] Sheikhhoseini R, Arab AM. Dry Needling in myofascial tracks in Non-Relaxing Pelvic Floor Dysfunction: A case study. J Bodyw Mov Ther. 2018 Apr;22(2):337-340. doi: 10.1016/j.jbmt.2017.09.016. Epub 2017 Sep 25. PMID: 29861229.