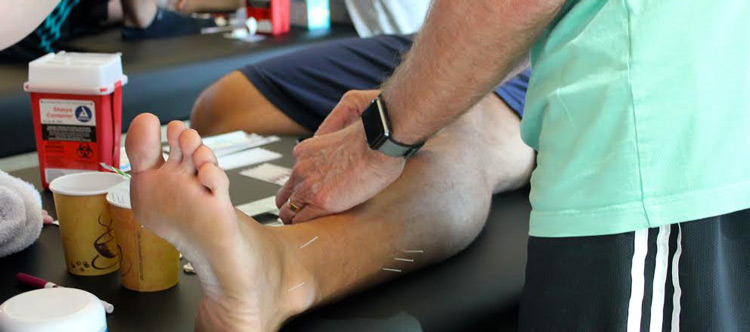
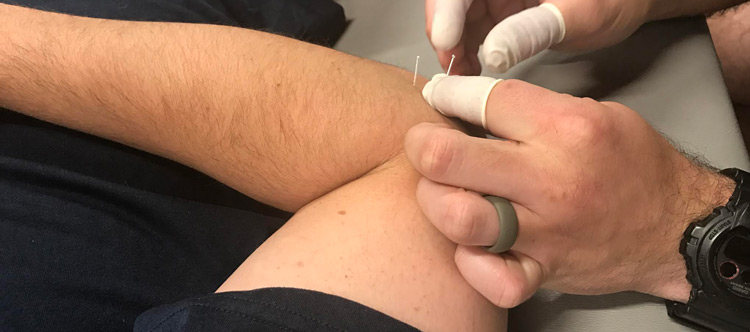
Dry needling has become one of my most used modalities in my clinical practice. The more I learn about it, the different techniques, the physiology and how to apply it to injury, performance and recovery the more I use it and the results keep improving. There are several misconceptions and general misinformation out there regarding dry needling. Hopefully I can shed some light on a few of these areas.
1) Dry Needling is NOT the same as acupuncture. We use the same tool (a fine, filament needle) but the similarities stop there. Acupuncture is rooted in Traditional Chinese Medicine. I have not spent any significant time studying meridians, pulse diagnosis, tongue diagnosis, Qi, yin/yang balance, or the 5 elements. What I HAVE done is spent well over 10,000 hours studying anatomy, physiology, musculoskeletal dysfunction, the nervous system, movement, palpation, medical and orthopedic assessment and injury. That (and my practice act in the state of which I am licensed) is what qualifies me (and my fellow PT’s, AT’s, DC’s, MD’s, and NP’s) to do dry needling. Everyone who uses a calculator is not an accountant, just like everyone who uses a filament needle is not an acupuncturist.
2) Dry needling treats absolutely nothing! Yet, it treats absolutely everything! The physiology that occurs when a needle is inserted into the tissue is extremely complicated but here are the three key things to remember: a) when a needle is inserted, CGRP (calcitonin gene-related peptide) is released. CGRP promotes vasodialation and formation of new blood vessels, thus facilitating repair after injury in the local tissue. b) Segmentally, the needle stimulates the small myelinated nerves in the body, triggering the release of enkephalin at the dorsal root ganglion of the spinal cord. Enkephalin blocks the transmission of pain at the spinal level the nerve originates from. c) Systemically, beta-endorphin is released in the brain (an opiate neuropeptide) and provides an overall analgesic effect in the body. This is the same opiate that is released when we receive spinal manipulation, and is in the same family as morphine. There you have it. A local, segmental and systemic response. THAT is why this modality is so powerful
3) Look at things objectively. Does your intervention produce immediate or latent responses? Are these responses measurable? With dry needling, my patient responses are objective and measurable. And they typically are significant.
4) There is no “one correct technique” in dry needling. Just like manual therapy and exercise prescription, there is an art to the use of dry needles in the human body. There are several techniques representing different theories and thoughts. None have been shown to be better or worse than others. They are simply different. As I have said before, if there was one correct way of doing things, we would all be doing it that way. Dry needling is no exception. There are many effective techniques and I always encourage students to learn multiple ways of doing things in order to see what fits best within their practice and philosophy.
5) Dry needling can be dangerous (driving a car can also be dangerous). Danger can be mediated with proper knowledge and care. It is important to respect the anatomy of the human body, know danger zones, and when dry needling is or is not indicated. Find a clinician who understands this and respects the invasive procedure. Appropriate universal precautions are always applied for the safety of the patient and the practitioner.
There is so much more to discuss I could write a book on it. But I don’t have to (yet)! There are some great books out there by authors including Jan Dommerholt and Adrian White. More and more peer-reviewed literature is being published and research is attempting to demystify some of the present unknowns.
This is an exciting time in the field of dry needling and I am so excited to be teaching more about this awesome modality. My upcoming courses are on my website structureandfunction.net . Hope to see some of you there!