There is increased discussion and debate regarding how needles can and should be used by health care practitioners. Some of this is a political issue, driven by state boards and their language used to describe and limit dry needling practice. Another discussion relates to the effectiveness and usefulness of trigger point dry needling. In this blog, I am going to illuminate these discussions in the hope of providing some insight into these issues of the dry needling squabble.
What is Trigger Point Dry Needling?
As early as the 1950s, practitioners began discussing trigger points in the literature and acknowledging the lack of attention paid to the muscle as a source of pain and dysfunction.1 Travell and Rinzler first used the term “myofascial trigger point” as a way of describing the nodules that can be present and refer pain to both muscle and overlying fascia.2 Current literature supports that trigger points are a common source of local and referred musculoskeletal pain and, more recently, can be classified as active or latent depending on their relationship with a patient’s pain and dysfunction.1,3 Active trigger points reproduce the pain symptoms experienced by an individual, while latent trigger points can be present and asymptomatic until pain is elicited upon provocation.1
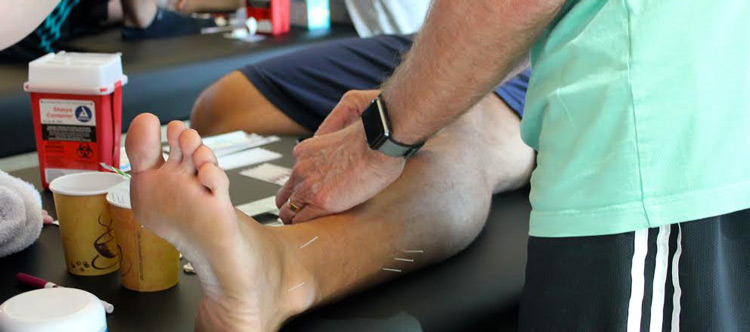
Trigger point dry needling is an invasive technique used to treat myofascial pain that uses a sterile, fine filiform needle without medication or injectate. This insertion of the needle into trigger points is accomplished by clinicians such as physical therapists, athletic trainers, and chiropractors with the goal of releasing/inactivating the trigger points, increasing blood flow, decreasing muscle tightness, and relieving pain.4,5 The clinician will insert the needle into the palpably painful nodule using a pistoning needling technique (similar to that of a sewing machine needle moving up and down). Elicitation of 1 or more local twitch responses is a stated goal of some dry needling practitioners and often benefits individuals with pain secondary to trigger points.6
Dry Needling for Myofascial Trigger Points
There is plenty of evidence to demonstrate that insertion of the needle into muscular trigger points works for pain relief. A recent clinical trial by Sanchez-Infante et al. shows what many past studies have found when looking at treatment for upper trapezius pain.7 Trigger point dry needling creates a local lesion and affects the mechanical properties of the local tissue. They discovered that trigger point dry needling decreased muscle tone at 30 minutes and 72 hours post needling. They concluded that trigger point dry needling to trigger points in the upper trapezius decreased dynamic stiffness, pain, tone, and contraction time after needling.7
Several systemic reviews have been completed looking at its effectiveness. Kietrys et al. did a review of trigger point dry needling for the management of pain in the upper quarter.8 The findings demonstrated that dry needling (when compared to sham or placebo treatment) provided evidence that dry needling can immediately decrease pain in patients with upper-quarter pain. They concluded that based on the best current available evidence (grade A), they recommend trigger point dry needling, compared to sham or placebo, for decreasing pain immediately after treatment and at four weeks in patients with upper-quarter MPS.8 Navaro-Santana et al. recently reviewed the effects of trigger point dry needling on lateral epicondylalgia of musculoskeletal origin.9 They reviewed seven studies, including 320 patients with lateral epicondylalgia. The meta-analysis found that trigger point dry needling reduced pain intensity and related disability with larger effect sizes than a comparison group. They also found that trigger point dry needling also increased pressure pain thresholds with large effect sizes and grip strength with small effect sizes compared to a comparison group. They concluded that low to moderate evidence suggests a positive effect of trigger point dry needling for pain, pain-related disability, pressure pain sensitivity, and strength in patients with lateral epicondylalgia of musculoskeletal origin. They also discuss that the literature demonstrates that the most significant effect was only of short duration. Lastly, Khan et al. reviewed trigger point dry needling of the lower extremity as a treatment strategy on pain and range of motion. They concluded that trigger point dry needling seemed effective in pain reduction related to lower extremity myofascial trigger points based on the best evidence available.10 These studies paint a quick picture of the effectiveness of trigger point approaches. However, most of these reviews had the caveat that there are a small number of high-quality randomized control trials published to date and that additional well-designed studies are needed to support trigger point dry needling.
What is the controversy?
The controversy lies in whether trigger point dry needling is the most effective way to apply needles to the body. Many have questioned the trigger point dry needling philosophy and underpinnings. Perhaps the starkest example is Dunning et al., who really drew attention to this application of needles and its effectiveness.4 Many question if trigger points can be accurately palpated and needled. In 2007 Tough et al. reviewed the criteria adopted by ‘‘experts’’ to diagnose myofascial trigger points.11 Their experts were defined as either researchers investigating trigger point pain syndrome or the ‘‘authority’’ the researchers cited as a source of reference for diagnosing trigger point pain syndrome. They reviewed and identified 19 different diagnostic criteria. The four most applied criteria were:
- ‘‘a tender spot in a taut band’’ of skeletal muscle.
- ‘‘patient pain recognition.’’
- ‘‘predicted pain referral pattern.’’
- ‘‘local twitch response.’’
They found no consistent pattern to the choice of specific diagnostic criteria or their combinations. However, one pair of criteria, ‘‘tender point in a taut band’’ and ‘‘predicted or recognized pain referral’’, were used by over half the studies. Interestingly, these studies cited publications by Travell and Simons as a principal authoritative source for trigger points. Despite this, the studies failed to apply similar diagnostic criteria or the criteria described by Travell and Simons. They concluded that further research is needed to test the reliability and validity of these diagnostic criteria. They also made the case that there is a need for greater transparency in research papers on how trigger points are defined and found until reliable diagnostic criteria have been established. The claims of effective interventions in treating the condition should be viewed with caution.11
Additional evidence questioning the trigger point dry needling approach relates to the lack of reliability in finding these trigger points.12,13 Myburgh et al. did a review that looked at the reproducibility of manual palpation in identifying trigger points.12 They found that the evidence suggested that, at best, moderate evidence could be found in the literature. From that literature, only local tenderness of the and pain referral of the gluteus medius and quadratus lumborum were found to be reproducible. They concluded that the methodologic quality of the studies of trigger points to establish trigger point reproducibility is generally poor. This calls into question if clinicians can even accurately find trigger points.12 This is similar to what Lucas et al. found in their study of reliability in finding trigger points.13
Another issue with trigger point dry needling is the notion that there needs to be a “twitch response” to have an effect or if that is indeed a goal of trigger point dry needling. Perreault et al. addressed this in a narrative review.6 They found that several studies show that eliciting a “twitch response” does not correlate with changes in pain and disability. They also state that multiple systematic reviews have failed to conclude whether the “twitch response” is relevant to the outcome of trigger point dry needling. They describe that needle winding without “twitch responses” is well supported in the literature, as it is linked to anti-nociception, tissue repair, and remodeling factors. They also state that physiologic changes in trigger points after needling may simply be related to local vasodilation. A “twitch response” during trigger point dry needling appears unnecessary for managing myofascial pain and is unrelated to many of the positive effects of trigger point dry needling.6
Conclusion
As you can see, there are multiple reasons for questioning the use of trigger point dry needling. Can trigger points be reliably found? Do we need to have a twitch response? Should that be the desired outcome? Or are the effects we see in the literature of trigger point dry needling just due to a local physiologic response to the lesion itself? At Structure & Function Education, we follow a comprehensive Pentamodal Method. One arm of the Pentamodal Method is a local approach, and this is where trigger point dry needling would fall within our methodology. We discuss these very local physiologic effects, and we needle locally when you want to change the local tissue. This is perhaps why trigger point dry needling works, and non-trigger point approaches such as in-situ needling (left in the tissue without needle manipulation) and winding are effective, as Perrault and colleges postulate. In fact, Butts et al. discuss that needling beyond the local trigger point is more efficacious in their narrative review. They concluded that trigger point dry needling with fast-in and fast-out pistoning maneuvers has not yet been shown to produce greater effects than in-situ needling at greater doses. They concluded that inserting multiple needles and leaving them in situ for 20-30 min durations has been shown to produce larger treatment effect sizes and longer-lasting outcomes than trigger point dry needling strategies.
If you want to learn more about trigger point dry needling and how to incorporate it into a more holistic approach to dry needling. Structure & Function Education’s Pentamodal Method of Dry Needling is for you. Enroll today in a Foundations in Dry Needling for Orthopedic Rehab & Sport Performance course at www.structureandfunction.net.
References:
- Shah JP, Thaker N, Heimur J, Aredo JV, Sikdar S, Gerber LH. Myofascial Trigger Points Then and Now: A Historical and Scientific Perspective. PM R. 2015;7(7):746-761. doi:10.1016/j.pmrj.2015.01.024
- Joseph Donnelly. Travell, Simons & Simons’ Myofascial Pain and Dysfunction : The Trigger Point Manual. Vol Third edition. Wolters Kluwer Health; 2019. Accessed January 10, 2022.
- Fernández-de-Las-Peñas C, Dommerholt J. International Consensus on Diagnostic Criteria and Clinical Considerations of Myofascial Trigger Points: A Delphi Study. Pain Med. 2018;19(1):142-150. doi:10.1093/pm/pnx207
- Dunning J, Butts R, Perreault T. On “Effectiveness of trigger point dry needling…” Cotchett MP, Munteanu SE, Landorf KB. Phys Ther. 2014;94:1083–1094. Physical Therapy. 2014;94(11):1677-1680. doi:10.2522/ptj.2014.94.11.1677
- Dunning J, Butts R, Mourad F, Young I, Flannagan S, Perreault T. Dry needling: a literature review with implications for clinical practice guidelines. Physical Therapy Reviews. 2014;19(4):252-265. doi:10.1179/108331913X13844245102034
- Perreault T, Dunning J, Butts R. The local twitch response during trigger point dry needling: Is it necessary for successful outcomes? Journal of Bodywork and Movement Therapies. 2017;21(4):940-947. doi:10.1016/j.jbmt.2017.03.008
- Sánchez-Infante J, Bravo-Sánchez A, Jiménez F, Abián-Vicén J. Effects of dry needling on mechanical and contractile properties of the upper trapezius with latent myofascial trigger points: A randomized controlled trial. Musculoskeletal Science and Practice
- Kietrys DM, Palombaro KM, Azzaretto E, et al. Effectiveness of Dry Needling for Upper-Quarter Myofascial Pain: A Systematic Review and Meta-analysis. Journal of Orthopaedic & Sports Physical Therapy. 2013;43(9):620-634. doi:10.2519/jospt.2013.4668
- Navarro-Santana MJ, Sanchez-Infante J, Gómez-Chiguano GF, et al. Effects of trigger point dry needling on lateral epicondylalgia of musculoskeletal origin: a systematic review and meta-analysis. Clin Rehabil. Published online June 23, 2020:026921552093746
- Khan I, Ahmad A, Ahmed A, Sadiq S, Asim HM. Effects of dry needling in lower extremity myofascial trigger points. J Pak Med Assoc. 2021;71(11):2596-2603. doi:10.47391/JPMA.01398
- Tough EA, White AR, Richards S, Campbell J. Variability of criteria used to diagnose myofascial trigger point pain syndrome–evidence from a review of the literature. Clin J Pain. 2007;23(3):278-286. doi:10.1097/AJP.0b013e31802fda7c
- Myburgh C, Larsen AH, Hartvigsen J. A systematic, critical review of manual palpation for identifying myofascial trigger points: evidence and clinical significance. Arch Phys Med Rehabil. 2008;89(6):1169-1176. doi:10.1016/j.apmr.2007.12.033
- Lucas NBs, Macaskill PB, Irwig LM, Moran RBs, Bogduk NM. Reliability of Physical Examination for Diagnosis of Myofascial Trigger Points: A Systematic Review of the Literature. [Review]. Clinical Journal of Pain. 2009;25(1):80-89. doi:10.1097/AJP.0b013e31