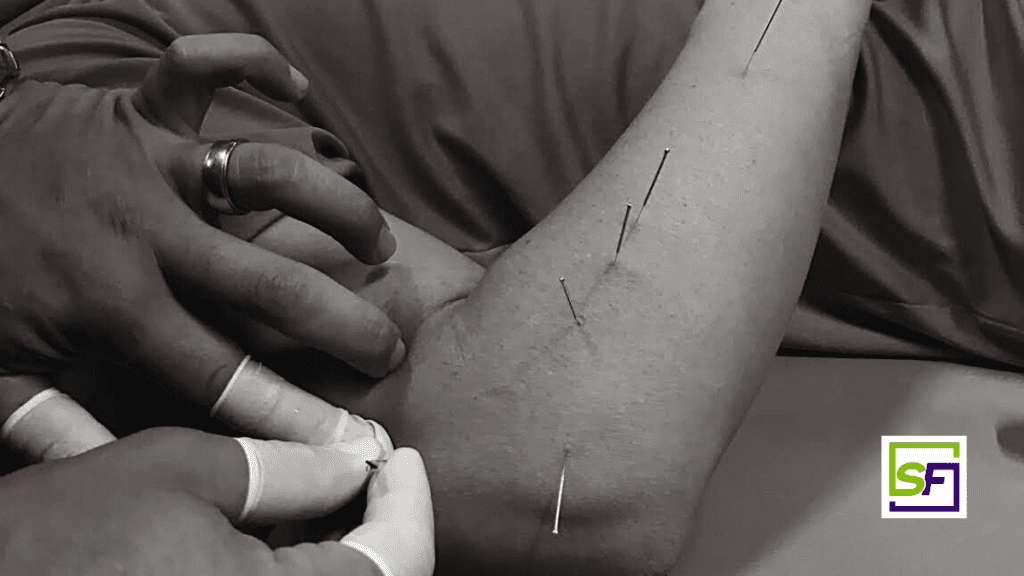
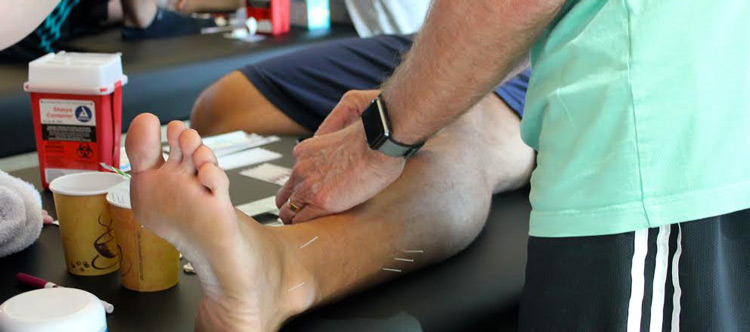
A question I often get asked by students in class is “can I use dry needling to help my post-stroke patients with spasticity?” The short answer is yes. There have been three articles recently written regarding the use of needling procedures to treat spasticity. These have sparked an interest in this area and I wanted to share these thoughts with our Structure & Function Education community.
Stroke & Spasticity:
According to the CDC, approximately 800,000 people have a stroke every year in the United States. The continued care of seven million stroke survivors costs the nation approximately $38.6 billion annually1. Spasticity is common after stroke, with the prevalence ranging from 30% to 80% of stroke survivors. The incidence of spasticity among paretic patients has been reported to be 27% at 1 month, 28% at 3 months, 23% and 43% at 6 months, and 34% at 18 months after stroke 2-3. It can lead to movement constraints and disability, if uncontrolled.
Pathophysiology:
Spasticity can be divided into two components: spasticity mediated by the neural reflex and spasticity due to muscle contracture, which is often referred to as non-reflex spasticity3. Although the underlying mechanisms are not well-understood, it may be due to disruption of the balance of supra-spinal inhibitory and excitatory sensory inputs directed to the spinal cord, leading to a state of disinhibition of the stretch reflex4. During the passive stretching of the muscles of a patient, there is sensory input from muscle spindles via primary group Ia afferent fibers to the spinal cord, and alpha-motoneurons are activated, with loss of supra-spinal inhibitory control, so that excessive muscle activation occurs5. Chronic spasticity can reduce the sarcomere number and increase the proportion of connective tissue in the muscle. The soft tissue change might cause the pulling forces to be transmitted more readily to the muscle spindles which can increase sensory input from muscle spindles and increase spasticity6-7.
The Case for Dry Needling Spasticity:
There is evidence for the use of dry needling to treat post-stroke spasticity8-13. When we turn to the acupuncture literature you see several systematic reviews that detail needling’s potential effects and that the data are getting better over time8-10. In 2014 Park et al.9, reviewed the acupuncture literature to determine the effect of acupuncture for spasticity in patients with stroke and concluded while there were some effects, the efficacy remains uncertain, primarily because of the poor quality of the available studies. They called for larger and more methodologically sound trials to definitively confirm or refute any effect of acupuncture as a treatment for spasticity after stroke9. Lim et al10., performed a meta-analysis showing that acupuncture or electroacupuncture significantly decreased spasticity after stroke. Their subgroup analysis showed that acupuncture significantly decreased wrist, knee, and elbow spasticity in post-stroke patients. They concluded that acupuncture could be effective in decreasing spasticity after stroke but long-term studies are needed to determine the longevity of treatment effects.
More recent evidence is provided by Zhu et al.8. In their review, they synthesized studies involving stroke, brain injury, spinal cord injury, cerebral palsy, and multiple sclerosis to give an overall picture of the effect and potential mechanisms of acupuncture on spasticity occurring after upper motor neuron lesions. They concluded that acupuncture has the therapeutic potential to help improve limb movement function and decrease the severity of spasticity. They concluded in particular, effectiveness with electroacupuncture. They state there is moderate-quality evidence suggesting that electroacupuncture combined with conventional routine care (pharmacological/rehabilitation) could reduce spasticity and improve motor function and activities in daily living after stroke8.
The electro-acupuncture literature also makes a strong case for adding electrical stim to your dry needling for spasticity11-12. Mukherjee et al.11, performed a study to quantitatively assess the change in spasticity of the impaired wrist joint in chronic stroke patients after electroacupuncture treatment. 2Hz stim was used for 30 minutes followed by therapeutic exercise. They found that a combination of electro-acupuncture and muscle-strengthening exercise for 6 weeks significantly reduced spasticity. The effect of spasticity reduction was consistent across different joint positions and different velocities of passive stretch11. Cai et al.12, reviewed the literature to evaluate the effects and safety of electroacupuncture for stroke patients with spasticity. They concluded that electroacupuncture combined with conventional routine care has the potential of reducing spasticity in the upper and lower limbs and improving overall and lower extremity motor function and activities of daily living for patients with spasticity, within 180 days post-stroke.
This brings us to the three very recent studies have provided additional evidence. Hernandez-Ortiz et al.13, investigated the effects of applying dry needling into a trigger point (TrP) or non-TrP area in people who have suffered a stroke and to investigate if the effects of dry needling are maintained at six-week follow-up. The effect of dry needling on muscle tone (spasticity) and upper extremity function is not related to its application in or outside of a TrP area. The effect of dry needling on shoulder pain was slightly superior when applied over a TrP in post stroke people. These effects were maintained six weeks after treatment. Ghannadi et al.14, designed a study to investigate the effects of deep dry needling on lower limb dysfunction in poststroke spastic patients. There were significant improvements in Modified Modified Ashworth Scale (MMAS) and functional tests (timed up and go test, 10-meter walk test), active ankle dorsiflexion range of motion (AROM), passive ankle dorsiflexion range of motion (PROM), and Barthel index. They concluded that deep dry needling decreases muscle spasticity and improves lower limb function and gait speed in post-stroke survivors.
Finally, an additional recent case study demonstrated FMRI evidence of how dry needling effects the CNS via fMRI14. Imaging was conducted in two steps before and immediately after DN using a task-based approach consisting of a right-hand thumb tapping task along with a physical examination before and 1.5 h after DN. DN was performed for 1 min on the dorsum of the hand, at the site of the proximal angle formed between the first and second metacarpal bones, using 1-inch stainless steel needles. The MMAS score for wrist flexors improved to “0” after DN. Active wrist extension ROM improved 10 degrees after DN. The hand Brunnstrom Recovery
Stage improved after DN. Baseline fMRI showed activation of the motor system during the finger-tapping task before the DN of the upper limb. The post-treatment fMRI revealed higher activation of both the affected and unaffected primary motor cortices, affected the primary somatosensory cortex, and affected the supplementary motor cortex. They concluded that improvements in hand function and active wrist extension might have been due to effective stimulation of the related motor cortex area after DN treatment.
All of this evidence demonstrates in its totality that the use of dry needling and dry needling with electric stimulation are potential “go to” treatments for post-stroke spasticity.
If you’re interested in learning how Structure & Function Education’s Pentamodal Method of Dry Needling can help you treat your patients with spasticity, enroll today at www.structureandfunction.net.
Brian Hortz, Ph.D., AT, SFDN
Director of Research and Education
Structure & Function Education
References
- Li S. Spasticity, Motor Recovery, and Neural Plasticity after Stroke. Front Neurol. 2017;8:120. Published 2017 Apr 3. doi:10.3389/fneur.2017.00120
- Brainin M, Norrving B, Sunnerhagen KS, et al. Poststroke chronic disease management: towards improved identification and interventions for poststroke spasticity-related complications. Int J Stroke. 2011;6(1):42-46. doi:10.1111/j.1747-4949.2010.00539.x
- Kuo, Chih-Lin, and Gwo-Chi Hu. “Post-stroke spasticity: a review of epidemiology, pathophysiology, and treatments.” International Journal of Gerontology 12.4 (2018): 280-284.
- Bhimani R, Anderson L. Clinical understanding of spasticity: implications for practice. Rehabil Res Pract. 2014;2014:279175. doi:10.1155/2014/279175
- Nardone A, Schieppati M. Reflex contribution of spindle group Ia and II afferent input to leg muscle spasticity as revealed by tendon vibration in hemiparesis. Clin Neurophysiol. 2005;116(6):1370-1381. doi:10.1016/j.clinph.2005.01.015
- Nielsen JB, Crone C, Hultborn H. The spinal pathophysiology of spasticity–from a basic science point of view. Acta Physiol (Oxf). 2007;189(2):171-180. doi:10.1111/j.1748-1716.2006.01652.x
- Mukherjee A, Chakravarty A. Spasticity mechanisms – for the clinician. Front Neurol. 2010;1:149. Published 2010 Dec 17. doi:10.3389/fneur.2010.00149
- Zhu, Yi, Yujie Yang, and Jianan Li. “Does Acupuncture Help Patients with Spasticity? A Narrative Review.” Annals of Physical and Rehabilitation Medicine 62, no. 4 (July 2019): 297–301. https://doi.org/10.1016/j.rehab.2018.09.010.
- Park, Si-Woon, Sook-Hee Yi, Jung Ah Lee, Pil Woo Hwang, Hyun Cheol Yoo, and Kyoung Sook Kang. “Acupuncture for the Treatment of Spasticity After Stroke: A Meta-Analysis of Randomized Controlled Trials.” The Journal of Alternative and Complementary Medicine 20, no. 9 (September 2014): 672–82. https://doi.org/10.1089/acm.2014.0097.
- Lim, Sung Min, Junghee Yoo, Euiju Lee, Hyun Jung Kim, Seungwon Shin, Gajin Han, and Hyeong Sik Ahn. “Acupuncture for Spasticity after Stroke: A Systematic Review and Meta-Analysis of Randomized Controlled Trials.” Evidence-Based Complementary and Alternative Medicine 2015 (2015): 1–12.https://doi.org/10.1155/2015/870398.
- Mukherjee, Mukul, Lisa K. McPeak, John B. Redford, Chao Sun, and Wen Liu. “The Effect of Electro-Acupuncture on Spasticity of the Wrist Joint in Chronic Stroke Survivors.” Archives of Physical Medicine and Rehabilitation 88, no. 2 (February 2007): 159–66. https://doi.org/10.1016/j.apmr.2006.10.034.
- Cai, Yiyi, Claire Shuiqing Zhang, Shaonan Liu, Zehuai Wen, Anthony Lin Zhang, Xinfeng Guo, Chuanjian Lu, and Charlie Changli Xue. “Electroacupuncture for Poststroke Spasticity: A Systematic Review and Meta-Analysis.” Archives of Physical Medicine and Rehabilitation 98, no. 12 (December 2017): 2578-2589.e4. https://doi.org/10.1016/j.apmr.2017.03.023.
- Hernández-Ortíz, Alma R, Raquel Ponce-Luceño, Carlos Sáez- Sánchez, Olga García-Sánchez, César Fernández-de-las-Peñas, and Ana I de-la-Llave-Rincón. “Changes in Muscle Tone, Function, and Pain in the Chronic Hemiparetic Shoulder after Dry Needling Within or Outside Trigger Points in Stroke Patients: A Crossover Randomized Clinical Trial.” Pain Medicine, June 3, 2020, pnaa132. https://doi.org/10.1093/pm/pnaa132.
- Ghannadi, Shima, Ardalan Shariat, Noureddin Nakhostin Ansari, Zahra Tavakol, Roshanak Honarpishe, Jan Dommerholt, Pardis Noormohammadpour, and Lee Ingle. “The Effect of Dry Needling on Lower Limb Dysfunction in Poststroke Survivors.” Journal of Stroke and Cerebrovascular Diseases, April 2020, 104814. https://doi.org/10.1016/j.jstrokecerebrovasdis.2020.104814.
- Mohammadpour, Fatemeh, Mohammad Ali Oghabian, Noureddin Nakhostin Ansari, Soofia Naghdi, and Jan Dommerholt. “Effects of Dry Needling on Post-Stroke Brain Activity and Muscle Spasticity of the Upper Limb: A Case Report.” Acupuncture in Medicine, June 12, 2020, 0964528420920294. https://doi.org/10.1177/0964528420920294.