In athletic and military populations ankle sprains are a common occurrence that could result in significant time loss due to injury. The National Electronic Injury Surveillance System (NEISS) estimated that between the years 2002 and 2006 that 3,140,132 ankle sprains reported to Emergency Departments in the United States. [1] It is estimated that the annual aggregate health-care cost of due to ankle sprains in the United States is $2 billion dollars. [1,2] The incidence of syndesmotic sprains varies from 1% to 11% of all ankle injuries. [3] High ankle sprains occur less in the general population, with a higher incidence in collision sports including football, ice hockey, and soccer with time loss from sport ranging from 0 to 137 days. [3] In athletics high ankle sprains do not resolve as quickly as lateral ankle sprains, and evidence of long- term disability has been shown in up 60% of patients. [1,2]
Mechanism
The most common mechanism for a high ankle sprain is forced external rotation of the foot and ankle while fixed or planted. [3,5,6] A second and less common mechanism is hyper dorsiflexion. [6] Separation of the mortise joint causes injury to the syndesmosis which can involve any or all of the following structures: anterior tibiofibular ligament; posterior tibiofibular ligament; interosseous ligament and interosseous membrane. [8] When these tissues are injured the amount of edema can vary. If the sprain is primarily in the distal portion of the tibiofibular ligament often will have localized swelling over the syndesmotic ligaments, however, when tears involve the interosseous membrane and/or the deltoid ligament there is an increase in swelling of the ankle and/or distal leg. [6]
Dry Needling High Ankle Sprains
Modulation of pain by needling the local tissues can occur through a couple of mechanisms. The first is segmental inhibition which is an updated version of the gate control theory of pain first published by Melzack and Wall in 1965. The hypothesis is activating A-Beta nerve fibers can lead to inhibition of pain transmission from A-Delta and C fibers at the dorsal horn. [7] The second is via the endogenous opioid system. There are three main groups of opioid peptides: beta endorphins, enkephalins, and dynorphins, and their mu, delta and kappa receptors distributed throughout the peripheral primary afferent terminals and areas of the central nervous systems related to nociception. [7] Opioids desensitize peripheral nociceptors, decrease proinflammatory cytokines in peripheral sites, and decrease cytokines and substance P in the spinal cord. [10] The addition of electric stimulation to the needles has been shown to increase these effects during treatment. Increasing evidence suggest that dry needling effects the HPA (Hypothalamic-Pituitary-Adrenal) axis mechanism which plays a role in homeostasis and how the body responds to stress. [9] A hypothesis suggests that the HPA axis is not only involved with the descending pain pathway but could share in an anti-inflammatory effect involving the neuroimmune pathways and the cholinergic anti-inflammatory mechanism. [9]
Dry Needling treatments can be an effective intervention when dealing with edema. Studies have shown that needling may increase muscle blood flow and oxygenation. [11] This is due to the presence of vasoactive chemicals such as CGRP and Substance P which are released when A-Delta and C fibers are stimulated. These substances have been shown to cause vasodilation in small vessels, increasing blow flow. [7] This increase in blood flow in peripheral areas can assist in the dissipation of edema.
Basic Intervention Using Aspects of the Pentamodal Method
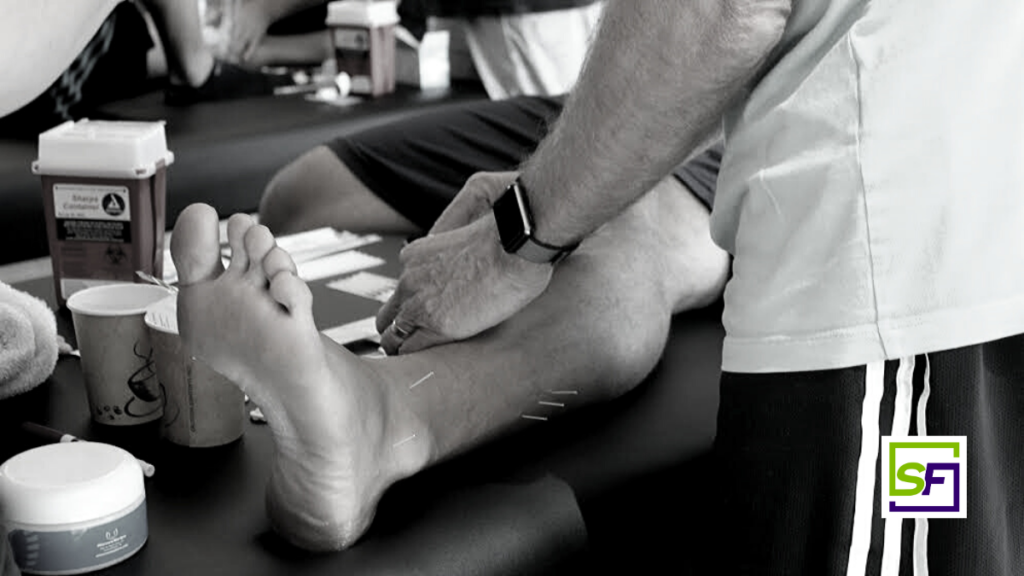
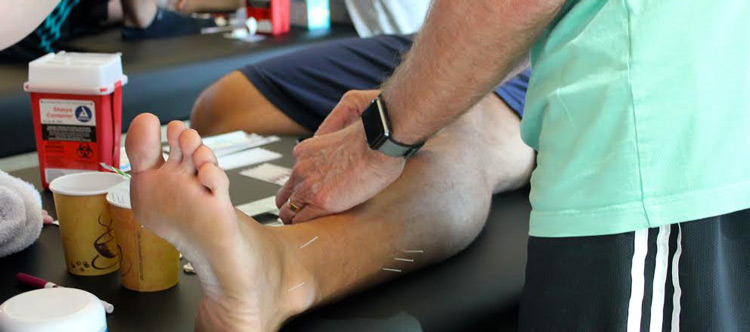
My initial treatment starts with the local involved tissues and the primary passive trigger points of the lower leg. In the syndesmosis itself, I will palpate distal to proximal the entire length of the painful area and insert needles every one to two finger-widths over that distance. In the most acute phase, I will start with 30mm needles and as the patient moves from acute to subacute I will increase the needle size to 50mm. I always add stim to this treatment starting at 2Hz for a treatment time of 20min. In addition to that, I have needles in the Deep Peroneal, Tibial, Saphenous and Common Peroneal PPTP’s. Clinically with this intervention, I have had a lot of success moving my athletes quicker toward resolution than before adding dry needles to my practice.
In the presence of swelling, I will add in the swelling protocol, filling the swollen area with 15mm needles every 1 finger width and leaving them in situ for 30 minutes.
I do not combine these two techniques on the same day as I believe it would overdose even my heartiest needling patient. Instead I apply each technique on a separate day followed by a day off from needling to allow the body to heal the lesions.
In particularly difficult cases, or if the local area is just too painful to needle I will fall back to needling centrally at L4, L5, S1 and apply 2Hz e-stim to those needles to activate the descending pain pathway.
Erik Marsh, SFDN, Associate Athletic Trainer
United States Air Force Academy
Instructor – Structure & Function Education
To learn more about the Pentamodal Method
If you’re interested in learning how Structure & Function Education’s Pentamodal Method of of dry needling can be used, enroll today in the Foundations in Dry Needling for Orthopedic Rehab & Sport Performance (SFDN1) at www.structureandfunction.net.
References:
- Waterman, Brian R. MD et al, The Epidemiology of Ankle Sprains in the United States. J Bone and Joint Surgery 2010; 92: 2279-84
- Waterman, Brian R. MD et al, Epidemiology of Ankle Sprain at the United States Military Academy. The American J of Sports Medicine 2010;130- 38:797-803
- Molinari, A., Stolley, M., Amendola, A. MD, High Ankle Sprains (Syndesmotic) in Athletes: Diagnostic Challenges and Review of the Literature. The Iowa Orthopaedic J 2009; 29: 130-138
- Miller, Bruce S. et al, Time to Return to Play after High Ankle Sprains in Collegiate Football Players: A Prediction Model 2012; Sports Health a Multidisciplinary approach 2012; Vol. 4 No. 6 504-509
- Nussbaum Eric D. et al, Prospective Evaluation of Syndesmotic Ankle Sprains without Diastasis, The American J of Sports Medicine, 2001; Vol 29 No1 31-35
- Williams, Glenn N. and Allen, Eric J. Rehabilitation of Syndesmotic (High) Ankle Sprains Sports Health 2010, Vol 2 No 6 460-470
- Cagnie, B. et al Physiologic Effects of Dry Needling, Curr Pain Headache Rep 2010; Vol 17 348-354
- Norkus, Susan A., Floyd, R., The Anatomy and Mechanisms of Syndesmotic Ankle Sprains. Journal of Athletic Training 2001; Vol 36 No1 68-73
- Warner, David S. MD Mechanisms of Acupuncture-Electroacupuncture on Persistent Pain. Anesthesiology, 2013; Vol 120 No 2 482-503
- Hwang, C. et al, Neural Substrates, Experiment Evidences and Functional Hypothesis of Acupuncture Mechanisms, Acta Neurologica Scandinavica, 2006 Vol 113 370-377
- Sandberg M., et al, Peripheral Effects of Needle Stimulation on Skin and Muscle Blood Flow in Fibromyalgia. European J of Pain. 2004; Vol 8 No 2 163-171