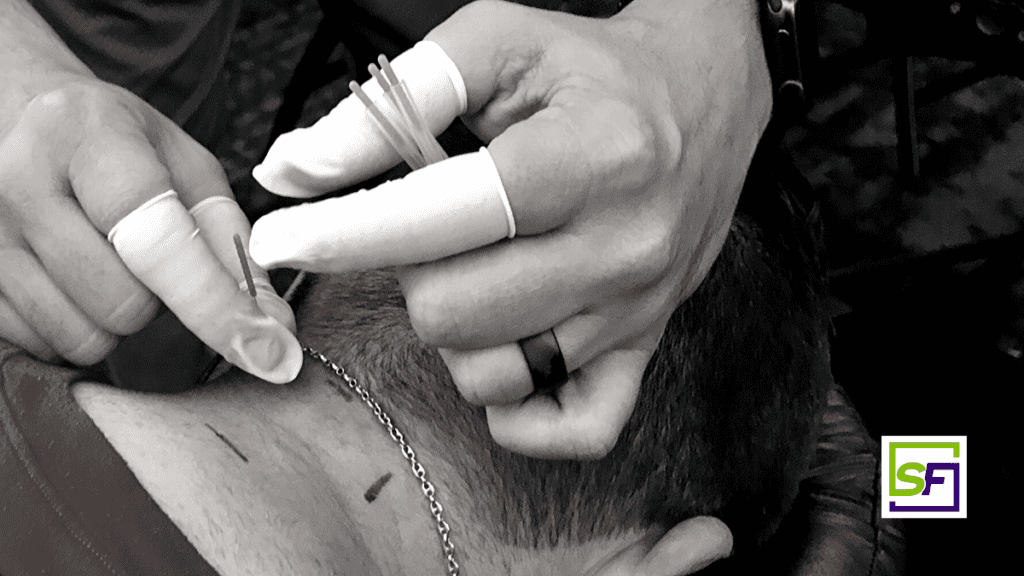
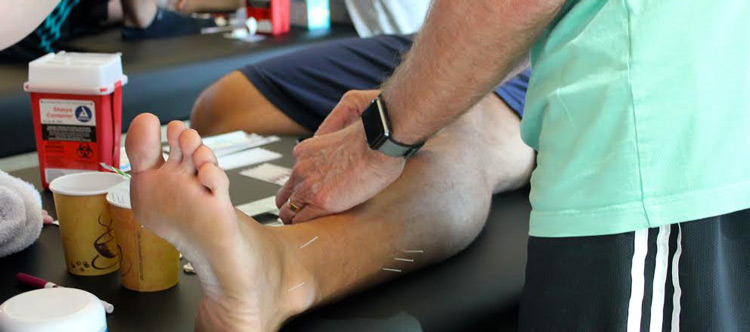
Treating Cervicogenic Headaches with Dry Needling and Manual Therapy
Cervicogenic headache refers to a headache of cervical origin1. The International Headache Society (IHS) has classified headaches as primary, where there is no other causative factor, or secondary, where the headache occurs in close temporal relationship to another disorder to which it is attributed2. A cervicogenic headache is a secondary headache caused by a disorder of the cervical spine and its component bone, nerve/nerve root, disc and/or soft tissue elements1,3–5. It is common to have referred pain perceived in the head from a source in the neck1,6,7. People with cervicogenic headaches often have a reduced range of motion of their neck and worsening of their headache with certain movements of their neck or pressure applied to certain spots on their neck. The headaches are often side-locked (on one side only), and the pain may radiate from the neck/back of the head up to the front of the head or behind the eye3,4,6. The headache may or may not be associated with neck pain. Diagnostic criteria have been established for cervicogenic headache, but its presenting characteristics may be difficult to distinguish from other headaches such as migraine or tension-type headache3.
Treatment of Cervicogenic Headaches via Dry Needling
A systematic review has investigated the effectiveness of dry needling and conventional physiotherapy in the management of cervicogenic headache or tension-type headache8. Two included clinical trials with tension-type headache participants demonstrated statistically significant improvements following dry needling8. Furthermore, one case report study with a cervicogenic headache female that was included in the systematic review showed significant improvement in pain and neck disability index after nine treatment sessions of dry needling combined with manual therapy8. Since that review, another author has published an article exploring superficial and deep dry needling for the treatment of cervicogenic headache9. The results of that study demonstrate the application of dry needling of suboccipital and upper trapezius muscles induces significant improvement of headache symptoms, functional rating index and range of motion in patients with cervicogenic headache. Additionally, they found that deep dry needling had greater effects on cervical range of motion and function9.
The acupuncture literature provides further evidence for the use of dry needling for the treatment of headaches. A systematic review of the literature investigated whether acupuncture is more effective than routine care than ‘sham’ acupuncture; and other interventions in reducing headache frequency in adults with episodic or chronic tension-type headache. The results indicated that acupuncture is effective for treating frequent episodic or chronic tension-type headaches, but further trials – particularly comparing acupuncture with other treatment options such as physical therapy, massage or exercise – are needed10. In another systematic review, the authors assessed the effectiveness of acupuncture in reducing headache frequency in patients with migraine. The results showed that there was consistent evidence that acupuncture provides additional benefit to the treatment of acute migraine attacks only or routine care11. Additionally, authors suggested that acupuncture is at least as effective as, or possibly more effective than, prophylactic drug treatment, and has fewer adverse effects11. The authors concluded that acupuncture should be considered a treatment option for patients with migraine willing to undergo this treatment11. Recently authors in the Cochrane Collaboration conducted a review of the effects of acupuncture for preventing tension-type headaches12. After searching for all relevant studies, they identified 2 studies comparing acupuncture to usual care, 4 studies comparing acupuncture to physiotherapy, massage or exercise treatment, and 7 studies comparing acupuncture to a sham (placebo) acupuncture treatment. They concluded that based on this evidence people who have frequent tension-type headaches will probably have slightly fewer headaches at 3-4 months after beginning a course of acupuncture. Specifically, people will probably have fewer ‘headache days’ per month, and probably more people will have half as many headaches12.
Treatment of Cervicogenic Headaches via Manipulation
Manual therapy can be very effective in conjunction with dry needling in the treatment of cervicogenic headaches13-14. The primary focus of manual therapy is to restore normal arthrokinematics of the cervical region with special attention to the upper cervical spine. For this discussion, we will define the upper cervical spine as the atlanto-occipital joint the axio-atlantal joint and the joints of the C2-3 segment. Restoring the function of these segments is paramount in finding a lasting solution to the cervicogenic headaches.
A very likely symptom generator can be an excessive extension of the occiput on the atlas in functional postures. This results in a compromise of the suboccipital space and can result in compression forces acting on the structures found in the suboccipital space. The most notable structures in question being the greater and lesser occipital nerves. These nerves can be part of the cause for the typical cervicogenic pain pattern radiating from the posterior aspect of the neck around the lateral aspect of the head just above the ear and terminating above the eyes. This is often termed a “ram’s horn” presentation. A common posture like “forward head posture,” where the occiput tends to rotate posteriorly on the atlas, often results in soft tissue and joint dysfunction that can be treated with manual therapy.
The research shows that with competent hands, manual therapy can be a very effective treatment modality the treatment of cervicogenic headaches by improving the function of the upper cervical spine. One randomized control trial found that manual therapy was effective in improving upper cervical mobility and providing immediate headache relief in patients with cervicogenic headaches13. Another randomized, double-blind placebo-controlled trial showed that improving C1-2 mobility via mobilizations reduced symptoms by 54% in individuals with cervicogenic headaches14. A randomized control trial of manual therapy in combination with exercise therapy found that manual therapy and exercise therapy were both effective in reducing headache symptoms, with a combination of the two being the most effective treatment. This approach demonstrated a statistically significant reduction in headache frequency and intensity that was sustained at the 12 month follow up assessment16. One pilot study of patients with cervicogenic headaches showed that addressing primary passive trigger points via manual therapy resulted in improved cervical range of motion, improved deep neck flexor function and a reduction in the presence of primary passive trigger points15.
Combined for Treatment of Cervicogenic Headaches
The research supports that dry needling and manual therapy are both proven techniques in the treatment of cervicogenic headaches8,9,12,14,15. Both techniques can stand alone as an effective approach however the combination of the two can be far superior in addressing cervicogenic headaches because of their unique and distinct target tissues17. Dry needling targeting soft tissue while manual therapy can be utilized to target joint dysfunctions. Dry needling is an excellent way to make manual therapy more effective and more comfortable for the patient.
Brian Hortz, PhD, AT, SFDN
Director of Research and Education – Structure & Function Education
Christian Compean PT, FAAOMPT
Instructor – Structure & Function Education
To learn more about the Pentamodal Method
If you’re interested in learning how Structure & Function Education’s Pentamodal Method of dry needling with cervical mobilization/manipulation can help you treat your patients with cervicogenic headaches, enroll today in a Foundations in Dry Needling for Orthopedic Rehab & Sport Performance and then the Advanced Cervical and Thoracic Spine course at www.structureandfunction.net.
References
- Page P. Cervicogenic headaches: an evidence-led approach to clinical management. Int J Sports Phys Ther. 2011;6(3):254–266.
- Headache Classification Committee of the International Headache Society (IHS) The International Classification of Headache Disorders, 3rd edition. Cephalalgia Int J Headache. 2018;38(1):1-211. doi:10.1177/0333102417738202
- Biondi DM. Cervicogenic headache: diagnostic evaluation and treatment strategies. Curr Pain Headache Rep. 2001;5(4):361-368. doi:10.1007/s11916-001-0026-x
- Chou LH, Lenrow DA. Cervicogenic headache. Pain Physician. 2002;5(2):215-225.
- Rana MV. Managing and treating headache of cervicogenic origin. Med Clin North Am. 2013;97(2):267-280. doi:10.1016/j.mcna.2012.11.003
- Biondi DM. Cervicogenic headache: mechanisms, evaluation, and treatment strategies. J Am Osteopath Assoc. 2000;100(9 Suppl):S7-14.
- Haldeman S, Dagenais S. Cervicogenic headaches: a critical review. Spine J Off J North Am Spine Soc. 2001;1(1):31-46. doi:10.1016/s1529-9430(01)00024-9
- France S, Bown J, Nowosilskyj M, Mott M, Rand S, Walters J. Evidence for the use of dry needling and physiotherapy in the management of cervicogenic or tension-type headache: A systematic review. Cephalalgia. 2014;34(12):994-1003. doi:10.1177/0333102414523847
- Sedighi A, Nakhostin Ansari N, Naghdi S. Comparison of acute effects of superficial and deep dry needling into trigger points of suboccipital and upper trapezius muscles in patients with cervicogenic headache. J Bodyw Mov Ther. 2017;21(4):810-814. doi:10.1016/j.jbmt.2017.01.002
- Nielsen A. Acupuncture for the Prevention of Tension-Type Headache (2016). Explore N Y N. 2017;13(3):228-231. doi:10.1016/j.explore.2017.03.007
- Linde K, Allais G, Brinkhaus B, et al. Acupuncture for the prevention of tension-type headache. Cochrane Pain, Palliative and Supportive Care Group, ed. Cochrane Database Syst Rev. April 2016. doi:10.1002/14651858.CD007587.pub
- Santesso N, Wieland LS. A Summary of a Cochrane Review: Acupuncture for the prevention of tension-type headache. Eur J Integr Med. 2016;8(4):324-325. doi:10.1016/j.eujim.2016.06.00
- Malo-Urries M, Tricas-Moreno JM, Estbanez-De Miguil E, Hidalgo-Garcia, Carrasco-Ubarren A, Cababillas, Barea S. Immediate Effect of Upper Cervical Translatoric Mobiliztion on the Cervical Mobility and Pressure Pain Threshold in Patients with Ecervicogenic Headache: A Randomized Controlled Trial. J Manipulative Physiol Ther. 2017 Nov-Dec; 40(9): 649–658. doi: 10.1016/j.jmpt.2017.07.007
- Toby Hall, Ho Tak Chan, Lene Christensen, Britta Odenthal, Cherie Wells, Kim Robinson. Efficacy of a C1-C2 self-sustained natural apophyseal glide (SNAG) in the management of cervicogenic headache. J Orthop Sports Phys Ther. 2007 Mar; 37(3): 100–107. doi: 10.2519/jospt.2007.2379
- Bodea-PradoG, Pecos-Martin D, et al. Manual treatment for cervicogenic headache and active trigger point in the sternocleidomastoid muscle: a pilot randomized clinical trial.
- Gwendolen Jull, Patricia Trott, Helen Potter, Guy Zito, Ken Niere, Debra Shirley, Jonathan Emberson, Ian Marschner, Carolyn Richardson. A randomized controlled trial of exercise and manipulative therapy for cervicogenic headache. Spine (Phila Pa 1976) 2002 Sep 1; 27(17): 1835–1843.
- Sillevis, Rob. “The Use of Dry Needling in Combination with Manual Therapy Techniques for a Patient with Cervicogenic Headache: A Case Report.,” 2011.