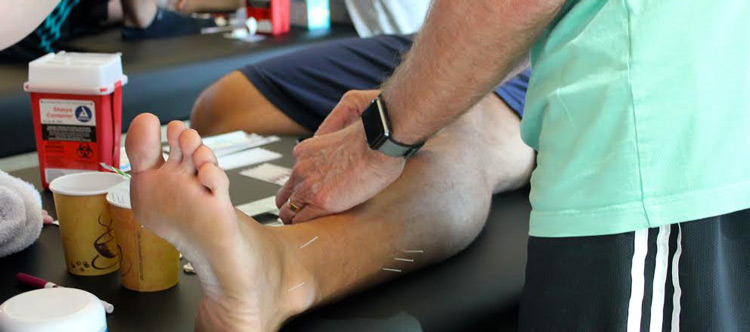
Top 3 Common Adverse Reactions When Being Dry Needled
Dry needling is a technique that involves the insertion of fine monofilament needles into anatomic structures to stimulate the healing process, relieve pain, and increase function. While dry needling is generally considered safe and effective, there are some potential adverse reactions when being dry needled that patients should be aware may occur. This blog will discuss the top adverse events that can occur when receiving dry needling.
Top 3 Adverse Reactions When Being Dry Needled:
- Bleeding: Dry needling involves the insertion of needles through the skin, which can sometimes pass through vessels, causing a small amount of blood to come to the skin’s surface upon the needle’s removal.
- Bruising: Due to the bleeding, sometimes it can cause small amounts of bruising in the area. This is more likely to occur in patients taking blood-thinning medications or having a bleeding disorder.
- Pain and Discomfort: Pain and discomfort are common adverse events associated with dry needling. Patients may experience a deep ache, muscle soreness, or a sharp, stabbing pain during and after the procedure. This is usually temporary and resolves within a few hours to a few days.
Data from two articles help us better understand the adverse reactions and how often they can occur when being dry-needled.1,2 Brady et al. designed a study to track mild and significant adverse reactions when performing dry needling.2 A prospective survey was undertaken consisting of two forms recording AEs. In the study, thirty-nine physiotherapists participated and provided 7629 dry needling treatments. 1463 (19.18%) mild adverse events were reported in the 7629 treatments. No significant AEs were reported giving an estimated upper-risk rate for significant AEs of less than or equal to 0.04%. They found that the most common adverse events included bruising (7.55% of patients), bleeding (4.65% of patients), pain during treatment (3.01% of patients), and pain after treatment (2.19% of patients).
Additionally, Boyce et al. studied adverse events as well. They recruited four hundred and twenty physical therapists to participate in a study of adverse events when dry needling.1 Participants recorded minor and major adverse events during 20,464 dry needling treatment sessions over six weeks. The top three minor adverse events were bleeding (occurring in 16% of patients), bruising (7.7% of patients), and pain during dry needling (5.9 % of patients). So these relatively minor events occur infrequently.
Additional Rare Adverse Reactions When Being Dry Needled
However, rare adverse reactions can occur, and patients should be informed of these and put them into proper perspective. These rare reactions include:
- Fainting: Some patients may experience fainting or dizziness during or after dry needling. This is more common in patients who are afraid of needles or have a fear of blood. According to Brady, this occurs .2% of the time and .78% of treatments in the Boyce article.
- Systemic Effects: Dry needling can sometimes cause systemic effects such as headaches, nausea, or dizziness. This is usually temporary and resolves within a few hours. This occurs (.14-.04%) of the time, according to Brady, and (.65-.46%) of treatments in the Boyce article—so fewer than 6 people per every 1000 treatments.
- Infection: Although rare, there is a risk of infection associated with dry needling. The needles used in dry needling are sterile, but if proper hygiene protocols are not followed, bacteria can enter the body and cause an infection. There were no infections in the study by Brady et al. and twice or .009% of treatments in the Boyce article. So very rare 2 in 100,000 treatments.
- Nerve Damage: Nerve damage is a potential risk associated with dry needling. If a needle is inserted too deeply or into the wrong area, it can damage a nerve and cause pain, numbness, or tingling in the affected area. There was 1 report of numbness.01% of treatments in the study completed by Brady et al. and 1 or .004% of treatments in the Boyce article. So very rare 4 in 100,000 treatments.
- Pneumothorax: Pneumothorax is a rare but potentially serious adverse event associated with dry needling. It occurs when a needle punctures the lung, causing air to leak into the chest cavity. This can cause chest pain and shortness of breath and, in severe cases, can be life-threatening. This is typically due to incorrect technique. Neither of the two studies that tracked adverse events had a pneumothorax reported. However, there have been some cases reported in the literature.3–5 Halle and Halle report the risk of pneumothorax with small gauge needles is less than one in 100,000 patients treated, and when it occurs, it can be a severe injury.6
It is important to note that while these adverse events are possible, they are relatively rare. Most patients undergoing dry needling experience mild to moderate discomfort that resolves quickly. However, discussing the potential risks and benefits of dry needling with your healthcare provider before undergoing the procedure is essential. If you experience any concerning symptoms after dry needling, such as persistent pain, bleeding, or signs of infection, seek medical attention immediately. Proper training can mitigate the risks associated with dry needling. If you are a patient, discuss the risks of this procedure with your therapist and discuss their training in dry needling your diagnosis. If you are a practitioner that wants to learn dry needling, you can find foundations courses near you; enroll in an open course today at www.structureandfunction.net.
Stay safe,
Brian Hortz
References
- Boyce D, Wempe H, Campbell C, et al. ADVERSE EVENTS ASSOCIATED WITH THERAPEUTIC DRY NEEDLING. Int J Sports Phys Ther. 2020;15(1):103-113. doi:10.26603/ijspt20200103
- Brady S, McEvoy J, Dommerholt J, Doody C. Adverse events following trigger point dry needling: a prospective survey of chartered physiotherapists. J Man Manip Ther. 2014;22(3):134-140. doi:10.1179/2042618613Y.0000000044
- Yamaguchi R, Makino Y, Torimitsu S, Chiba F, Kihara Y, Iwase H. Fatal bilateral pneumothoraces after electroacupuncture treatment: A case report and literature review. J Forensic Sci. n/a(n/a). doi:10.1111/1556-4029.14874
- Bagcier F, Yurdakul OV. Letter to the Editor regarding: A case with iatrogenic pneumothorax due to deep dry needling. Radiol Case Rep. 2020;15(11):2329-2330. doi:10.1016/j.radcr.2020.09.006
- Lee SS. Acupuncture-induced hemopneumothorax: a case report. Acupunct Med. Published online August 19, 2022:09645284221117843. doi:10.1177/09645284221117843Halle JS, Halle RJ. PERTINENT DRY NEEDLING CONSIDERATIONS FOR MINIMIZING ADVERSE EFFECTS – PART ONE. Int J Sports Phys Ther. 2016 Aug;11(4):651-62. PMID: 27525188; PMCID: PMC4970854.
- Halle JS, Halle RJ. PERTINENT DRY NEEDLING CONSIDERATIONS FOR MINIMIZING ADVERSE EFFECTS – PART ONE. Int J Sports Phys Ther. 2016 Aug;11(4):651-62. PMID: 27525188; PMCID: PMC4970854.